The Vagus Nerve and Deep Pressure: How DPS Affects Your Nervous System
The vagus nerve is why deep pressure calms the body. Learn how it works, how to stimulate it, and what it means for anxiety and sleep.
The DPS Editorial Team
Editorial Team ·
📖 Table of Contents
Affiliate Disclosure: As an Amazon Associate I earn from qualifying purchases. Some links on this page are affiliate links — if you buy through them, we receive a small commission at no extra cost to you. This never influences which products we recommend. Full disclosure policy →
If you want to understand why weighted blankets, firm hugs, and compression vests actually calm the nervous system — the vagus nerve is the answer.
What Is the Vagus Nerve?
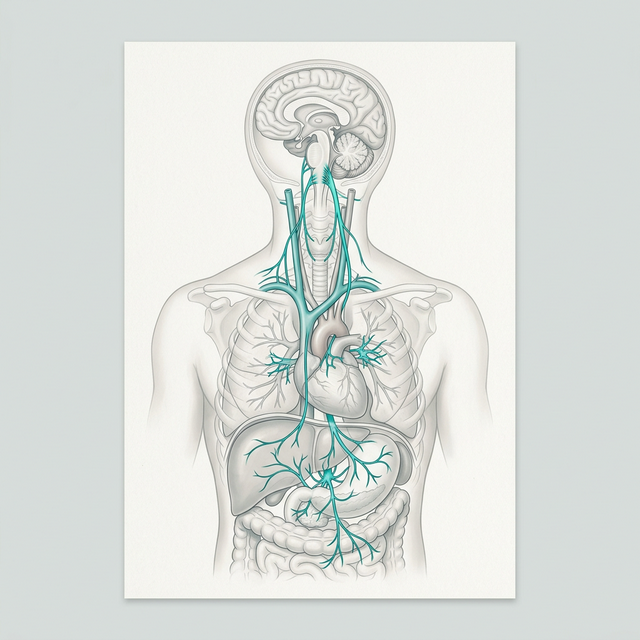
The vagus nerve is the tenth cranial nerve and the longest, most complex nerve in the body. It runs from the brainstem down through the neck, into the chest (where it connects to the heart and lungs), and continues into the abdomen (where it connects to the digestive system, liver, and kidneys).
The term comes from the Latin word for “wandering” — which describes its path through the body perfectly.
The vagus nerve is the primary driver of the parasympathetic nervous system — the “rest and digest” system. When vagal tone is high, the body is calm: heart rate is low, breathing is slow and deep, digestion functions normally, and the mind is clear.
When vagal tone is low or the vagus is disengaged, the sympathetic “fight or flight” system dominates: heart rate rises, breathing quickens, digestion stops, and the nervous system scans for threats.
How Deep Pressure Activates the Vagus Nerve
Deep pressure stimulation activates the vagus nerve through mechanoreceptors — specialized sensory nerve endings in the skin and underlying tissue that detect firm, sustained pressure.
When these mechanoreceptors are activated by sustained pressure (a weighted blanket, a compression vest, a firm hug), they send signals through the peripheral nervous system to the brainstem, where the vagal nucleus is located.
This afferent (incoming) signal tells the brainstem: “The body is receiving safe, organized touch.” The vagus nerve responds by increasing parasympathetic output — the neurological equivalent of applying the brakes to a revved-up stress response.
The result is measurable and rapid:
- Heart rate decreases (the vagal brake at work)
- Heart Rate Variability (HRV) increases — a key marker of autonomic flexibility and resilience
- Cortisol drops — studies show up to 31% reduction
- Digestive activity resumes — you may notice your stomach “settling” during deep pressure
- Breathing slows and deepens automatically — driven by diaphragm relaxation
Polyvagal Theory and Deep Pressure
Psychiatrist Stephen Porges developed Polyvagal Theory — a framework that describes three distinct states of the autonomic nervous system and how they relate to safety and social engagement. In this framework:
- Ventral Vagal (safe, connected): The healthy social engagement state. The ventral branch of the vagus supports calm, attentive interaction with others.
- Sympathetic Mobilization (fight or flight): Activated when we perceive threat. Heart rate up, muscles ready for action.
- Dorsal Vagal Shutdown (freeze, collapse): The most primitive response — numbness, dissociation, collapse.
Deep pressure stimulation appears to specifically activate the ventral vagal pathway — moving the nervous system toward safety and social engagement rather than just suppressing sympathetic response. This is one reason why DPS is effective not just for anxiety but also for social engagement in autism, where the ventral vagal system may be underactive.
Vagus Nerve Stimulation vs. Deep Pressure: How They Compare
Medical vagus nerve stimulation (VNS) uses an implanted device to deliver electrical impulses directly to the vagus nerve — used clinically for epilepsy, depression, and inflammatory conditions. It’s invasive and prescription-only.
Deep pressure stimulation provides a gentler, non-invasive version of vagal activation through the sensory surface of the body. It’s less powerful than medical VNS but accessible, safe, and usable daily.
Other non-invasive vagal activation methods — cold water on the face, deep slow breathing (especially long exhales), singing or humming — work through different branches of the same pathway.
What High Vagal Tone Means for Health
Sustained vagal activation through regular DPS practice (consistent weighted blanket use, regular massage, compression garments) may contribute to increased baseline vagal tone — a measure of how active and flexible the parasympathetic system is at rest.
High vagal tone is associated with:
- Lower baseline anxiety
- Better emotion regulation
- Improved recovery from stress
- Better sleep quality
- Reduced inflammatory markers
- Better heart rate variability
This is why OTs recommend consistent daily use of DPS tools rather than purely reactive use during crisis moments. The more regularly the vagus nerve receives “safe” signals, the higher the baseline tone and the more resilient the nervous system becomes.
Frequently Asked Questions
Can I stimulate my vagus nerve at home without special equipment?
Yes. Effective vagal stimulation methods include: deep slow breathing with long exhales (4 counts in, 8 counts out), cold water on the face or neck, singing or humming, gargling with water, and deep pressure (firm self-massage, weighted blankets, compression). Even basic deep breathing with a weighted lap pad combines two methods simultaneously.
How quickly does vagal activation from deep pressure take effect?
Measurable heart rate reduction typically begins within 2–5 minutes of sustained deep pressure. Subjective calm arrives slightly later — usually 5–15 minutes. The effect is real-time, not cumulative — though regular practice builds baseline vagal tone over weeks and months.
Is Polyvagal Theory scientifically accepted?
Polyvagal Theory is widely used in clinical settings and has been influential in trauma therapy and OT. Some neuroscientists critique specific anatomical claims in the theory. For practical purposes — the three-state model and the role of the vagus nerve in safety and calm — the clinical evidence strongly supports the core concepts, even if the theoretical framework continues to evolve.
Can deep pressure heal a chronically dysregulated nervous system?
It can contribute meaningfully. DPS is a bottom-up regulatory tool — it works through the body to influence the brain. For chronic dysregulation (complex trauma, long-term anxiety disorders), DPS is most effective when combined with top-down approaches: trauma-informed therapy, CBT, and nervous system education. No single tool heals a traumatized nervous system alone.

The DPS Editorial Team
Editorial Team
The DeepPressureStimulation.com Editorial Team researches and writes about deep pressure stimulation, weighted blankets, and sensory tools. We are not licensed occupational therapists or medical professionals. All content is based on peer-reviewed research, published clinical guidelines, and reputable health sources. Always consult a qualified healthcare provider before starting any new therapy.
Stay Informed, Stay Calm
Get science-backed articles on deep pressure therapy, weighted blankets, and sensory tools delivered to your inbox. No spam — just calm.
📬 No spam, ever. Unsubscribe anytime.